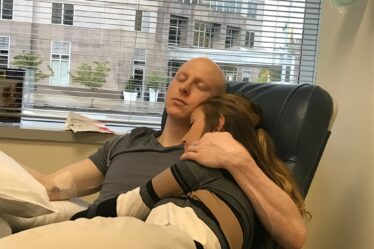
A guest blog from Vicki Campana, an ovarian cancer survivor

By Vicki Campana,
A note from Jenna Lindman about Vicki.
Vicki Campana is a 41-year-old ovarian cancer fighter who currently lives in Cleveland, OH. She is a manager in Business Intelligence Operations, and enjoys photography in her free time. Vicki was diagnosed with cancer in 2015. At the time, she was struggling with some pain and fertility issues and had sought out help from doctors who had trouble diagnosing her issues at first. What they thought was a cyst on her ovary turned out to be much more serious. Vicki has now been in remission for three years, her journey with has continued. After beating her own cancer, her brother was diagnosed with Hodgkin’s lymphoma and recently completed treatment. She stayed strong for him, caretaking and supporting him as much as she could. She adopted the attitude, “Hope anchors the soul,” which helped her get through her journey.
Vicki stresses the importance of being thorough with the questions you ask regarding your own health, she states, “Take time to grieve the situation, take time to heal physically and ask lots of questions. We have to be our own advocates. No two people are alike when it comes to any type of diagnosis, but doctors treat us like we are. There are text book treatments that they follow, but sometimes there is more to the story, and we need to push to make sure we have all of the information available to us.”She has shared her journey with us today. Vicki, thank you so much for telling us your story, and opening up the conversation about ovarian cancer and fertility.
Hello, my name is Vicki Campana and I am 41 years old.
In 2012 I had pain in my left side that was causing discomfort, and no one could figure out what was causing it. I had a colonoscopy, scan, chiropractic adjustments and an ultrasound by my gynecologist. Luckily multiple chiropractic adjustments got my hip back in line and relieved my pain. During my ultrasound, they did discover a dermoid cyst on my right ovary, so the Dr. decided to monitor it. 2013 another gynecologist agreed it was a dermoid and that we would monitor for any changes. I stopped birth control after my wedding in 2011 and hadn’t been able to conceive yet. She recommended a fertility specialist, but I decided to wait. February 2014, I became pregnant. We were beyond excited that it had finally happened. We were going to be parents. At my 12-week checkup, it was confirmed that I had a miscarriage.

January 2015 there did not appear to be any change over the last 3 years to the cyst. We met with the fertility specialist that year and when he reviewed my history, he decided he wanted a current ultrasound done. He agreed it was a dermoid cyst, but it appeared that it may be slightly larger than images seen just a few months before. We removed the cyst to help increase our chances of becoming pregnant and free up room with the ovary.
July 31st, 2015 the fertility doctor removed the cyst. On August 10th, he told me that we needed to put things on hold. Behind the cyst there was a small GCT (Granulosa Cell Tumor), stage 1 Ovarian cancer. Approximately 5% of ovarian cancers are this type. I had gone alone that day because my husband had started a new job. I decided to not contact him at work and had to sit with this all day. After a brief update on his first day, I blurted out I had cancer.
I met a gynecologic oncologist and decided we would remove the ovary/fallopian tube on the right side, de-bulk and confirm my stage. I was told that 95% of patients are done at this point, the cancer is removed, and you would be monitored throughout the years for re-occurrence.

That is not what happened for me. Microscopic traces of the cancer were found on my left abdomen wall, meaning the cancer had leaked outside the right ovary and had made its way to the opposite side of my body. My left ovary was clear, so they kept it. I was moved up to stage 3A. Although the traces of cancer were microscopic, it was recommended that we be aggressive and treat this with six rounds of chemotherapy, Carboplatin and Taxol.
We decided to proceed with In vitro fertilization (IVF) retrieving eggs from the good ovary before chemo, fertilizing them and freezing the embryos until we were ready to proceed again. They extracted 8 eggs and fertilized them, but our worst fears were confirmed when they told us none of them survived. I had put my body through so much in 12 weeks, but we had to take the chance. We hoped and prayed that the left ovary would successfully survive chemo
I had many signs of my ovarian cancer– bloating, feeling full, the cyst, but everyone assumed it was the dermoid cyst and nothing more was needed than monitoring its size. I wish the gynecologists had been a bit more aggressive. Not every case is the same. Were they not listening to me? I didn’t know any better at the time to keep pushing and none of them wanted to dig further.
Treatment started October 2015. I received chemo every three weeks, finishing February 2016. I worked through my treatments. I should have let my body rest and taken the time to heal physically and mentally, but I decided I was pushing through. I was allergic to one of the chemos, so I was put on a steroid reducing the additional side effects that it was causing. I gained over 20lbs almost instantly. I lost my hair before my second round. I had pain in my knees, after every session and still suffer from joint pain.

I pushed for genetic testing even though this was deemed a non-genetic cancer. I was only positive for one gene – ATM. It was currently on the watch list. There were cases where they believed breast cancer was connected to it, but not enough to deem it a concern.

December 2016-February 2017, we unsuccessfully tried Intrauterine insemination (IUI). We were about to start IVF again and were notified that the ATM gene was officially connected to breast cancer. Then we found out my grandmother had breast cancer, and her mother had passed from it years ago. I was told I had 20-60% chance of getting breast cancer sometime in my lifetime, based on history, my ovarian cancer and now the gene. July 2017, we removed my other ovary. This reduced my chances of ovarian cancer again, and I would no longer be able to have try to have children naturally and risk passing on the gene.

September 2017, I had a double mastectomy reducing my chances of breast cancer to less than 1%. We went in planning for one surgery, direct to implant. I had 3 surgeries due to complications and lack of healing between then and April 2018. This was not a free boob job. I no longer look the same, I struggle to feel like myself. I know I made the right decision to prevent something before it could happen.
To monitor my ovarian cancer, I have a blood test every 3 months looking at Inhibin A & B, and CA125. Since my ovaries are removed, those levels should be around 0, so we will hopefully know quickly if there is ever a return of my cancer. Since I had my breasts removed, I do not need to monitor for breast cancer. There is no breast tissue left.
I am being hopeful and optimistic as I move forward, but I am not who I once was. Cancer changed me. Physically and emotionally. Those that have gone through chemo experience similar and different side effects. In the 1st year after chemo ended, I occasionally had heart palpitations. I experience dizziness often, odd aches and I still tire easily. I am reminded every day that I had cancer. I choose to share my experiences so that I can help educate others, as well as open the door to conversations.